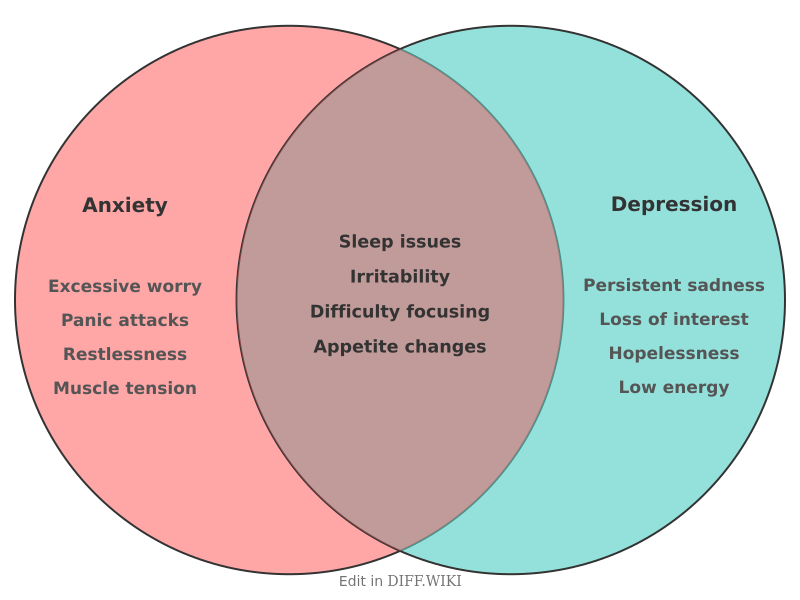
Differences between anxiety- and depression
Contents
Anxiety vs. depression[edit]
Anxiety and depression are mental health conditions classified by the American Psychiatric Association in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5). Although they are distinct clinical diagnoses, they frequently occur together. Statistics from the National Alliance on Mental Illness (NAMI) indicate that approximately 60% of people with depression also experience symptoms of an anxiety disorder.
Anxiety is primarily characterized by persistent worry, fear, and physiological hyperarousal. In contrast, depression is defined by a pervasive low mood, a loss of interest in activities (anhedonia), and a sense of hopelessness.
Comparison table[edit]
| Feature | Anxiety | Depression |
|---|---|---|
| Primary emotion | Fear, apprehension, or dread | Sadness, emptiness, or hopelessness |
| Temporal focus | Future-oriented (worry about what might happen) | Past or present-oriented (rumination on failures or current state) |
| Physiological state | Hyperarousal, racing heart, sweating, and tremors | Low energy, fatigue, and psychomotor retardation |
| Sleep patterns | Difficulty falling asleep due to racing thoughts | Waking up too early or sleeping excessively (hypersomnia) |
| Cognitive style | Overestimating risk or threat | Underestimating self-worth or the possibility of improvement |
| Physical symptoms | Muscle tension, gastrointestinal distress, and headaches | Significant changes in weight or appetite and chronic pain |
| Primary drive | Urge to escape or avoid perceived danger | Lack of motivation or drive to engage with the world |
Clinical distinctions[edit]
The "tripartite model" is often used by clinicians to differentiate between the two states. According to this framework, both conditions share "negative affect," which refers to general emotional distress. However, physiological hyperarousal is specific to anxiety, while low positive affect (the inability to feel pleasure) is specific to depression.
Anxiety disorders, such as Generalized Anxiety Disorder (GAD) or Panic Disorder, involve a "fight-or-flight" response that is triggered even when no immediate threat is present. This leads to physical tension and mental alertness. Major Depressive Disorder (MDD) involves a "shut down" response. Patients with depression often describe a feeling of being "heavy" or "numb" rather than "wired" or "tense."
Diagnostic overlap and comorbidity[edit]
Because the two conditions share a genetic basis and involve similar neurotransmitter systems—specifically serotonin and norepinephrine—they are often treated with similar medications, such as selective serotonin reuptake inhibitors (SSRIs). Cognitive behavioral therapy (CBT) is also a standard treatment for both.
Despite these similarities, the focus of therapy differs based on the diagnosis. Therapy for anxiety often centers on exposure to feared stimuli and reducing avoidance behaviors. Therapy for depression often emphasizes behavioral activation, which involves scheduling activities to increase the patient's exposure to positive reinforcement and social interaction.
References[edit]
- American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
- National Alliance on Mental Illness. (2023). "Anxiety Disorders."
- Clark, L. A., & Watson, D. (1991). "Tripartite model of anxiety and depression: Psychometric evidence and taxonomic implications." Journal of Abnormal Psychology, 100(3), 316–336.
- Mayo Clinic. (2022). "Depression and anxiety: Can I have both?"