Differences between Osteoarthritis and Rheumatoid Arthritis
Contents
Osteoarthritis and rheumatoid arthritis comparison[edit]
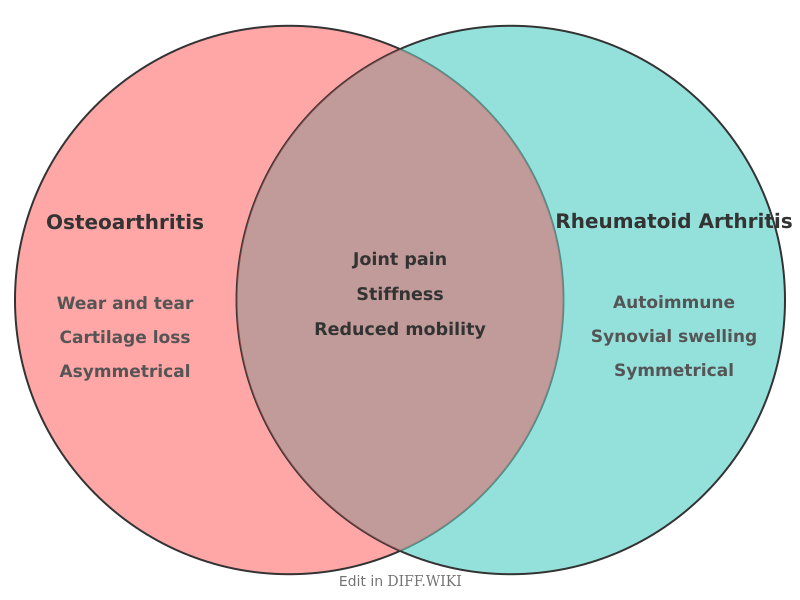
Osteoarthritis (OA) and rheumatoid arthritis (RA) are chronic conditions that affect the joints. While both diseases result in pain and decreased mobility, they have different underlying causes and clinical presentations. Osteoarthritis is primarily a degenerative condition caused by the breakdown of joint cartilage over time. Rheumatoid arthritis is a systemic autoimmune disease where the body's immune system attacks the synovium, which is the lining of the membranes surrounding the joints.[1]
Comparison table[edit]
| Feature | Osteoarthritis (OA) | Rheumatoid arthritis (RA) |
|---|---|---|
| Primary cause | Cartilage degeneration (mechanical) | Autoimmune response (inflammatory) |
| Age of onset | Usually later in life (age 50+) | Can occur at any age (often 30–60) |
| Speed of onset | Gradual, over years | Rapid, over weeks or months |
| Joint distribution | Asymmetric (often one side) | Symmetric (affects both sides equally) |
| Morning stiffness | Lasts less than 30 minutes | Lasts longer than 60 minutes |
| Common joints | Knees, hips, lower back, fingers | Wrists, knuckles, feet, ankles |
| Systemic symptoms | Absent | Fatigue, fever, weight loss |
| Blood markers | No specific markers | Elevated RF, anti-CCP, and ESR |
Pathophysiology and symptoms[edit]
The mechanical nature of osteoarthritis means that pain usually worsens after physical activity or at the end of the day. In OA, the protective cartilage that cushions the ends of the bones wears down, leading to bone-on-bone friction. This process often results in the formation of bone spurs, known as osteophytes. In the hands, these appear as bony enlargements called Heberden's nodes (at the distal joints) and Bouchard's nodes (at the middle joints).[2]
Rheumatoid arthritis involves a chronic inflammatory process. The immune system targets the joint lining, causing it to thicken and eventually destroy the cartilage and bone within the joint. Because RA is a systemic disease, it can affect organs beyond the musculoskeletal system, including the lungs, heart, and eyes. Patients with RA often experience "flares," which are periods of increased disease activity, followed by periods of remission.[3]
Diagnosis and management[edit]
Physicians diagnose osteoarthritis primarily through physical examinations and imaging. X-rays may show joint space narrowing or the presence of bone spurs. Blood tests in OA patients typically show normal levels of inflammatory markers. Treatment focuses on symptom relief through weight management, low-impact exercise, and analgesics like acetaminophen or nonsteroidal anti-inflammatory drugs (NSAIDs).
Diagnosis of rheumatoid arthritis requires a combination of clinical assessment and laboratory testing. High levels of rheumatoid factor (RF) or anti-citrullinated protein antibodies (anti-CCP) in the blood support an RA diagnosis. C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) tests indicate the level of inflammation in the body. Management of RA often involves disease-modifying antirheumatic drugs (DMARDs) or biologic agents to slow disease progression and prevent permanent joint deformity.[4]
References[edit]
- ↑ Mayo Clinic. (2023). "Arthritis."
- ↑ Arthritis Foundation. "Osteoarthritis vs. Rheumatoid Arthritis: What’s the Difference?"
- ↑ National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2023). "Rheumatoid Arthritis."
- ↑ Johns Hopkins Arthritis Center. "Rheumatoid Arthritis Signs and Symptoms."