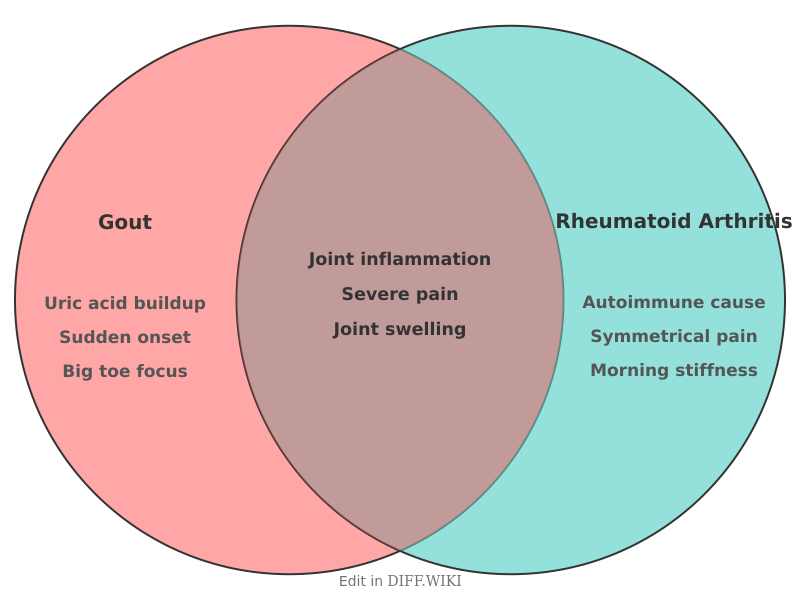
Differences between Gout and Rheumatoid Arthritis
Contents
Comparison of gout and rheumatoid arthritis[edit]
Gout and rheumatoid arthritis (RA) are two distinct types of inflammatory arthritis. Although both conditions cause joint pain, swelling, and potential long-term disability, they differ in their underlying causes, clinical presentation, and management strategies. Gout is a metabolic disorder caused by the accumulation of monosodium urate crystals in the joints, while RA is a chronic autoimmune disease where the immune system attacks the synovium (the lining of the membranes that surround the joints).[1][2]
Comparison table[edit]
| Feature | Gout | Rheumatoid arthritis |
|---|---|---|
| Primary cause | Uric acid crystal deposits | Autoimmune response |
| Onset of symptoms | Sudden (often overnight) | Gradual (weeks to months) |
| Symmetry | Asymmetric (one joint at a time) | Symmetric (affects both sides of body) |
| Common initial joint | Big toe (podagra) | Small joints of hands and feet |
| Morning stiffness | Brief (less than 30 minutes) | Prolonged (over 60 minutes) |
| Systemic symptoms | Fever (rarely) | Fatigue, weight loss, low-grade fever |
| Diagnosis markers | Urate crystals in synovial fluid | RF and anti-CCP antibodies |
| Gender prevalence | More common in men | More common in women |
| Treatment focus | Uric acid reduction | Immune system suppression |
Clinical characteristics[edit]
Gout typically presents as an acute monoarthritis, meaning it affects a single joint during a flare. The most frequent site of an initial attack is the first metatarsophalangeal joint. These flares are often characterized by rapid onset of intense pain, redness, and warmth. Pain levels generally peak within 12 to 24 hours of onset. Between flares, patients may experience long periods without symptoms, although chronic gout can lead to tophi (visible lumps of urate crystals) and permanent joint damage.[3]
Rheumatoid arthritis is a polyarthritis, usually involving multiple joints in a symmetric pattern. If the knuckles on the right hand are inflamed, the same knuckles on the left hand are typically affected as well. RA symptoms include persistent joint stiffness that is most severe in the morning or after periods of inactivity. Unlike gout flares, RA is a progressive condition that requires continuous management to prevent the destruction of bone and cartilage.[4]
Diagnosis and management[edit]
Doctors distinguish between the two conditions using patient history, physical examination, and laboratory tests. A definitive diagnosis of gout is made by performing an arthrocentesis (joint fluid aspiration) to identify needle-shaped urate crystals under a polarized light microscope. Blood tests for hyperuricemia (high uric acid) are common but not always conclusive, as uric acid levels can fluctuate during an attack.[5]
The diagnosis of RA involves blood tests for rheumatoid factor (RF) and anti-cyclic citrullinated peptide (anti-CCP) antibodies. Imaging such as X-rays or ultrasound is used to detect joint erosions and narrowing of the joint space. Management of RA relies on disease-modifying antirheumatic drugs (DMARDs) and biologics to slow disease progression. Gout management focuses on lifestyle changes and medications like allopurinol to lower serum urate levels.[6]
References[edit]
- ↑ Mayo Clinic. (2023). Gout. Mayo Foundation for Medical Education and Research.
- ↑ Mayo Clinic. (2023). Rheumatoid arthritis. Mayo Foundation for Medical Education and Research.
- ↑ Arthritis Foundation. (n.d.). Gout vs. Rheumatoid Arthritis: What’s the Difference?
- ↑ American College of Rheumatology. (2021). Rheumatoid Arthritis.
- ↑ American College of Rheumatology. (2020). Management of Gout.
- ↑ NHS. (2023). Arthritis.