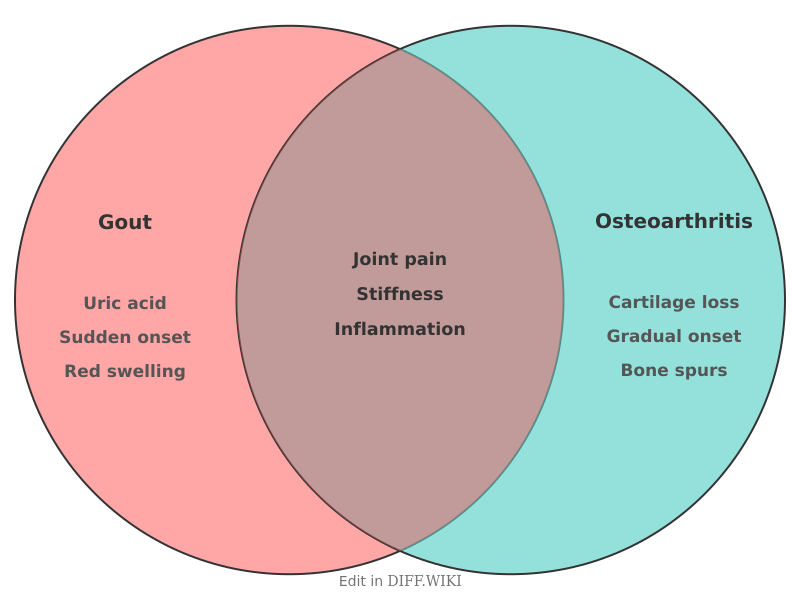
Differences between Gout and Osteoarthritis
Contents
Gout and osteoarthritis[edit]
Gout and osteoarthritis are two of the most prevalent forms of arthritis, yet they result from different biological processes. Gout is a metabolic condition characterized by the sudden deposition of monosodium urate crystals within joints, leading to acute inflammation. Osteoarthritis is a chronic degenerative disease involving the mechanical breakdown of articular cartilage and underlying bone. While both conditions cause significant joint pain and physical limitation, their clinical presentation, risk factors, and long-term management strategies are distinct.
Pathophysiology[edit]
The primary cause of gout is hyperuricemia, a state where uric acid levels in the blood exceed the limit of solubility. This leads to the formation of needle-like crystals in the synovial fluid. Uric acid is a byproduct of purine metabolism; high levels often stem from either overproduction or, more commonly, decreased renal excretion.
In contrast, osteoarthritis involves the progressive "wear and tear" of joint structures, though current research also identifies low-grade inflammatory components. Factors such as aging, joint injury, and obesity contribute to the loss of cartilage, which reduces the cushioning between bones. As the cartilage thins, the body may respond by forming osteophytes, or bone spurs, which further restrict movement and cause pain.
Clinical presentation[edit]
Gout typically presents as "attacks" or flares. These are sudden episodes of intense pain, often beginning at night. The most common site is the first metatarsophalangeal joint (the base of the big toe), a condition known as podagra. Affected joints usually appear red, swollen, and are extremely tender to the touch.
Osteoarthritis develops gradually over years. Pain is usually described as a dull ache that worsens with activity and improves with rest. Morning stiffness is common but typically lasts less than 30 minutes, unlike inflammatory conditions like rheumatoid arthritis. OA frequently affects weight-bearing joints such as the knees and hips, as well as the distal joints of the fingers.
Comparison table[edit]
| Feature | Gout | Osteoarthritis |
|---|---|---|
| **Primary cause** | Uric acid crystal accumulation | Degeneration of joint cartilage |
| **Onset** | Sudden, acute flares | Gradual, chronic progression |
| **Typical age** | Usually 30–50 in men; post-menopause in women | Usually over age 50 |
| **Inflammation** | High (redness, heat, swelling) | Low to moderate |
| **Common joints** | Big toe, ankles, knees | Knees, hips, spine, fingers |
| **Systemic links** | Diet, alcohol, kidney function | Obesity, joint trauma, genetics |
| **Diagnostic test** | Synovial fluid analysis (crystals) | Physical exam and X-ray (joint space narrowing) |
| **Pain trigger** | High-purine foods, dehydration | Physical activity, weather changes |
Diagnosis and management[edit]
Physicians confirm a gout diagnosis by extracting synovial fluid from the affected joint and examining it under a polarized light microscope to identify urate crystals. Blood tests for uric acid can be suggestive but are not definitive, as levels may fluctuate during an acute attack. Management involves nonsteroidal anti-inflammatory drugs (NSAIDs) or colchicine for acute flares, and urate-lowering therapies like allopurinol for long-term prevention.
Osteoarthritis is primarily diagnosed through physical examination and imaging. X-rays may show a narrowing of the space between bones or the presence of bone spurs. Management focuses on symptom control and functional maintenance. This includes physical therapy, weight loss to reduce joint load, and analgesics. In advanced cases where conservative treatments fail, joint replacement surgery may be required.
References[edit]
- Richette, P., & Bardin, T. (2010). "Gout". The Lancet, 375(9711), 318-328.
- Glyn-Jones, S., et al. (2015). "Osteoarthritis". The Lancet, 386(9991), 376-387.
- American College of Rheumatology. (2020). "Guidelines for the Management of Gout".
- Hunter, D. J., & Bierma-Zeinstra, S. (2019). "Osteoarthritis". New England Journal of Medicine, 380(18), 1745-1757.