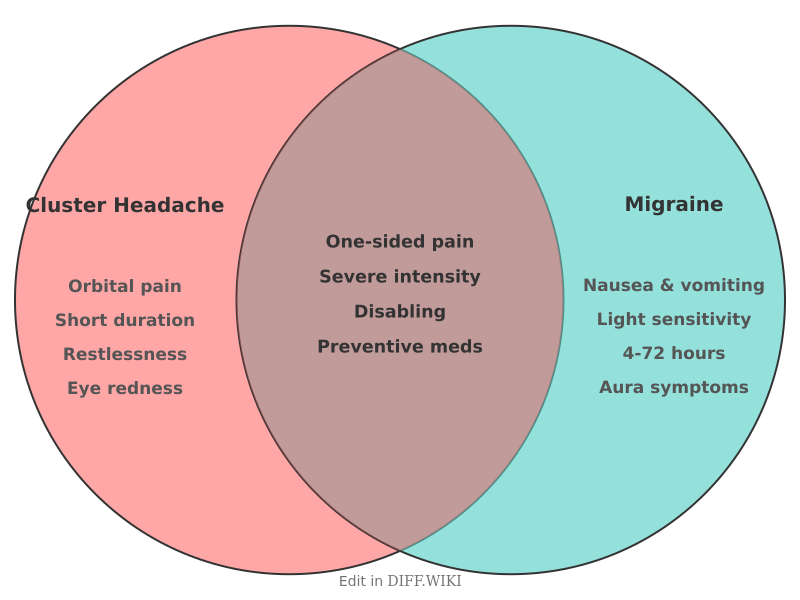
Differences between Cluster Headache and Migraine
Contents
Cluster headache vs. migraine[edit]
Cluster headache and migraine are distinct primary headache disorders characterized by recurrent bouts of moderate to severe pain. Although both conditions involve the trigeminal vascular system, they differ in their clinical presentation, duration, and associated autonomic or systemic symptoms. Accurate diagnosis is necessary because the pharmacological treatments for each condition, such as abortive oxygen therapy for cluster headaches or triptans and calcitonin gene-related peptide (CGRP) inhibitors for migraines, are not always interchangeable.[1]
Comparison table[edit]
| Feature | Cluster headache | Migraine |
|---|---|---|
| Pain location | Strictly unilateral; usually around or behind one eye. | Often unilateral but can shift sides or become bilateral. |
| Pain quality | Sharp, stabbing, or "boring" sensation. | Pulsating or throbbing. |
| Attack duration | 15 to 180 minutes. | 4 to 72 hours. |
| Frequency | 1 to 8 attacks per day during a "cluster" period. | Varies widely; often several times per month. |
| Patient behavior | Restlessness; pacing or rocking to cope with pain. | Preference for lying still in a dark, quiet room. |
| Gender ratio | More common in men. | More common in women. |
| Autonomic signs | Tearing, nasal congestion, or drooping eyelid on the affected side. | Usually absent; nausea and vomiting are more common. |
| Triggers | Alcohol or strong smells during a cluster bout. | Stress, hormonal changes, specific foods, or weather changes. |
Clinical presentation[edit]
Migraine is often preceded by a prodrome or an aura. The aura consists of reversible neurological symptoms, such as visual flashes, blind spots, or tingling in the extremities, which typically develop over five to twenty minutes.[2] During the headache phase, movement often worsens the pain. Migraine patients frequently report sensitivity to light (photophobia) and sound (phonophobia).
In contrast, cluster headache is known for its "alarm clock" regularity, with attacks often occurring at the same time each day or night. The pain is described as one of the most severe sensations known to medical science. Unlike migraine patients, those experiencing a cluster attack are typically unable to stay still. They may pace the floor or exhibit physical agitation. Cluster headaches are categorized by the presence of cranial autonomic symptoms on the same side as the pain, such as miosis (constriction of the pupil), ptosis (drooping of the eyelid), or rhinorrhea (runny nose).[3]
Pathophysiology and cycles[edit]
The temporal patterns of these disorders serve as a primary diagnostic marker. Migraines can occur at any time and may be chronic or episodic. Cluster headaches often follow seasonal cycles, appearing for several weeks or months followed by periods of remission that can last for years. Research suggests the hypothalamus, which regulates the body's biological clock, plays a more significant role in the initiation of cluster headaches than in migraines.[4]