Differences between Asthma and COPD
Contents
Comparison of asthma and COPD
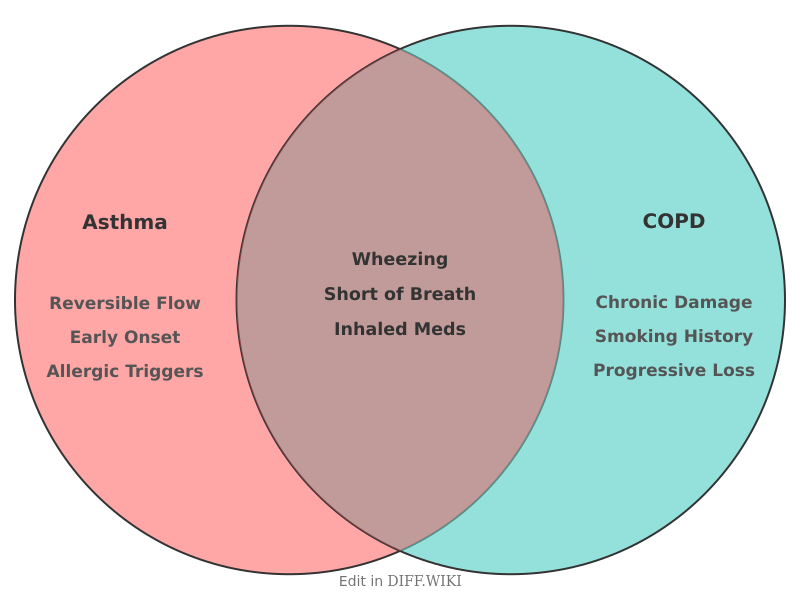
Asthma and chronic obstructive pulmonary disease (COPD) are chronic conditions characterized by inflammation of the airways and obstruction of airflow. While these diseases share several clinical symptoms, such as coughing, wheezing, and shortness of breath, they are distinct in their etiology, pathophysiology, and clinical progression.
The primary distinction lies in the reversibility of airflow limitation. In asthma, the narrowing of the airways is usually intermittent and can be reversed, either spontaneously or with medical treatment. In COPD, the airflow limitation is persistent and typically worsens over time. This obstruction is generally caused by a combination of small airway disease (obstructive bronchiolitis) and parenchymal destruction (emphysema), the relative contributions of which vary between individuals.[1]
Comparison table
| Feature | Asthma | COPD |
|---|---|---|
| Typical age of onset | Usually childhood or adolescence | Usually over age 40 |
| Smoking history | Not a primary cause; may be a trigger | Present in the vast majority of cases |
| Airflow limitation | Largely reversible | Not fully reversible |
| Primary inflammatory cells | Eosinophils, mast cells, Th2 cells | Neutrophils, macrophages, CD8+ T cells |
| Typical symptoms | Variable; asymptomatic between attacks | Persistent and progressive |
| Family history | Common (atopy/allergy) | Less common (except Alpha-1 antitrypsin deficiency) |
| Primary treatment focus | Inhaled corticosteroids (anti-inflammatory) | Bronchodilators and risk factor reduction |
Pathophysiology and inflammatory patterns
The underlying cellular mechanisms differ significantly between the two conditions. Asthma is frequently associated with an underlying allergic component, known as atopy. The inflammation in the asthmatic airway involves the activation of Th2 lymphocytes, which stimulate eosinophils and mast cells. This process leads to airway hyperresponsiveness to various triggers, such as pollen, pet dander, or cold air.
In contrast, COPD is primarily an inflammatory response to the chronic inhalation of noxious particles or gases, most commonly cigarette smoke. In developing countries, exposure to biomass fuels for cooking and heating is a significant cause. The inflammatory response in COPD involves neutrophils, macrophages, and CD8+ T lymphocytes. Over time, this chronic inflammation leads to structural changes including the narrowing of the small airways and the destruction of alveoli, which reduces the surface area available for gas exchange.[2]
Diagnosis and clinical presentation
Spirometry is the objective test used to confirm the diagnosis of both diseases. Physicians measure the forced expiratory volume in one second (FEV1) and the forced vital capacity (FVC). In asthma, an improvement in FEV1 of more than 12% and 200 mL following the administration of a bronchodilator indicates significant reversibility. In COPD, a post-bronchodilator FEV1/FVC ratio of less than 0.70 confirms the presence of persistent airflow limitation.
Clinical history also provides diagnostic clues. Asthma patients often report that their symptoms are worse at night or in the early morning. COPD patients more commonly report chronic productive cough and exertional dyspnea that progresses gradually over several years. While some patients exhibit features of both conditions, a phenomenon previously termed "Asthma-COPD Overlap Syndrome," clinical guidelines now emphasize identifying the dominant underlying condition to guide therapy.[3]
References
- ↑ Global Initiative for Chronic Obstructive Lung Disease. (2024). Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease.
- ↑ Postma, D. S., & Rabe, K. F. (2015). The Asthma–COPD Overlap Syndrome. New England Journal of Medicine, 373(13), 1241–1249.
- ↑ Global Initiative for Asthma. (2023). Global Strategy for Asthma Management and Prevention.