Differences between Gout and Pseudogout
Contents
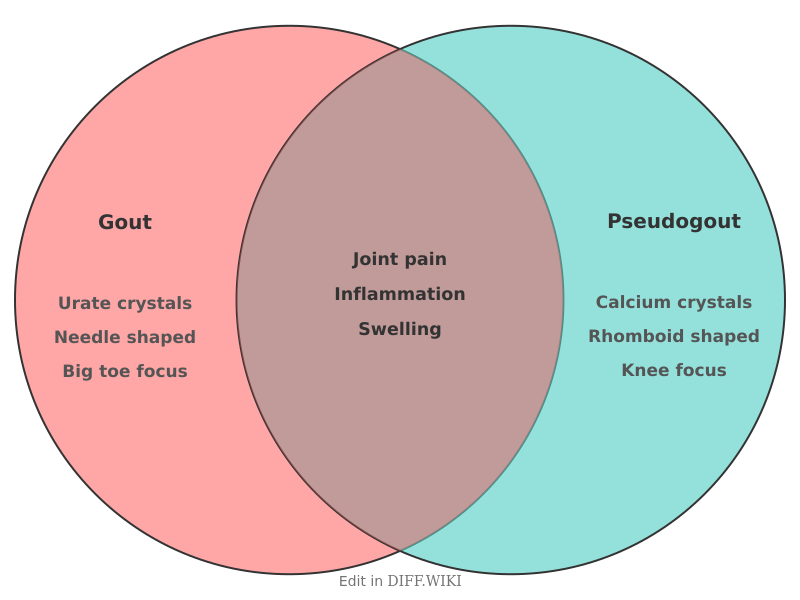
Gout vs. pseudogout
Gout and pseudogout are inflammatory joint diseases caused by the deposition of mineral crystals in synovial fluid and surrounding tissues. While both conditions present with sudden onset pain, swelling, and warmth in the joints, they differ in their chemical composition, typical locations, and long-term management. Gout results from the accumulation of monosodium urate (MSU) crystals, whereas pseudogout—medically termed calcium pyrophosphate deposition (CPPD) disease—is caused by calcium pyrophosphate dihydrate crystals.
Comparison of gout and pseudogout
| Feature | Gout | Pseudogout (CPPD) |
|---|---|---|
| Crystal composition | Monosodium urate (MSU) | Calcium pyrophosphate dihydrate |
| Crystal shape | Needle-shaped | Rhomboid or brick-shaped |
| Birefringence | Strongly negative | Weakly positive |
| Most common joint | First metatarsophalangeal (big toe) | Knee |
| Typical demographics | Middle-aged men; postmenopausal women | Elderly populations (over 65) |
| Primary risk factors | Diet (purines), alcohol, obesity, diuretics | Aging, hyperparathyroidism, hemochromatosis |
| Blood markers | Elevated serum uric acid (hyperuricemia) | Normal uric acid; possible low magnesium |
| Radiographic findings | "Punched-out" bone erosions, tophi | Chondrocalcinosis (cartilage calcification) |
| Acute treatment | NSAIDs, colchicine, corticosteroids | NSAIDs, colchicine, joint aspiration |
Pathophysiology and diagnosis
Gout is closely associated with hyperuricemia, a state where uric acid levels in the blood exceed the limit of solubility. This occurs either through the overproduction of uric acid or, more commonly, decreased excretion by the kidneys. When concentrations are high enough, crystals precipitate in joints, triggering an immune response. Gouty attacks often occur at night and can be triggered by dehydration, certain medications, or the consumption of high-purine foods such as organ meats and shellfish.
Pseudogout is primarily a disease of aging. The mechanism involves the breakdown of adenosine triphosphate (ATP) in the joint cartilage, leading to increased levels of pyrophosphate. This pyrophosphate then combines with calcium to form crystals. Unlike gout, pseudogout does not have a direct link to dietary intake, but it is frequently seen in patients with underlying metabolic disorders like hyperparathyroidism or low blood magnesium levels.
Diagnosis for both conditions requires arthrocentesis, a procedure where synovial fluid is aspirated from the affected joint and examined under a compensated polarized light microscope. In gout, the needle-like crystals appear bright yellow when aligned parallel to the axis of the compensator (negative birefringence). In pseudogout, the rhomboid crystals appear blue when aligned parallel (positive birefringence).
Management and prognosis
Acute management for both conditions focuses on reducing inflammation. Long-term management for gout often involves urate-lowering therapy, such as allopurinol or febuxostat, to prevent future attacks and the formation of tophi (visible lumps of urate crystals). Because pseudogout is often secondary to other conditions or aging, management focuses on treating the underlying metabolic cause and using prophylactic low-dose colchicine for patients with frequent recurrences.
References
- ↑ Kuo, C. F., et al. (2015). "Gout: epidemiology and risk factors." Nature Reviews Rheumatology, 11(11), 649-662.
- ↑ Rosenthal, A. K., & Ryan, L. M. (2016). "Calcium Pyrophosphate Deposition Disease." New England Journal of Medicine, 374(26), 2575-2584.
- ↑ Zhang, W., et al. (2011). "EULAR recommendations for calcium pyrophosphate deposition. Part II: Management." Annals of the Rheumatic Diseases, 70(4), 571-575.
- ↑ Richette, P., & Bardin, T. (2010). "Gout." The Lancet, 375(9711), 318-328.